Chronic Diseases Which Impact Women More Or Differently Than Men

There are many chronic diseases which impact women more, differ from the same diseases affecting men, or are diagnosed in women less frequently than in men. These diseases include cardiac diseases, autoimmune diseases, osteoporosis, Alzheimer’s disease, and metabolic issues. Chronic diseases of women affect millions of individuals each year. Such factors as hormones, genes, and decades of research, mostly devoted to men, contribute to the problem. Thus, chronic illnesses of women are often diagnosed later, treated with medications which do not work efficiently in women, and lead to complications. This paper will examine five major conditions, the problem of research bias, and possible solutions which may be used in the future.
Cardiovascular Disease
Heart disease is the top cause of death for women, yet doctors still miss it more often in them than in men. Women are about 50 percent more likely to receive a wrong initial diagnosis during a heart attack. The classic symptom most people picture—crushing chest pain—is common in men. In women, signs can be subtler: shortness of breath, nausea, vomiting, extreme tiredness, jaw or back pain, or a vague feeling that something is wrong. These symptoms get mistaken for anxiety, acid reflux, or just stress. Women’s chronic diseases often include these hidden heart risks.
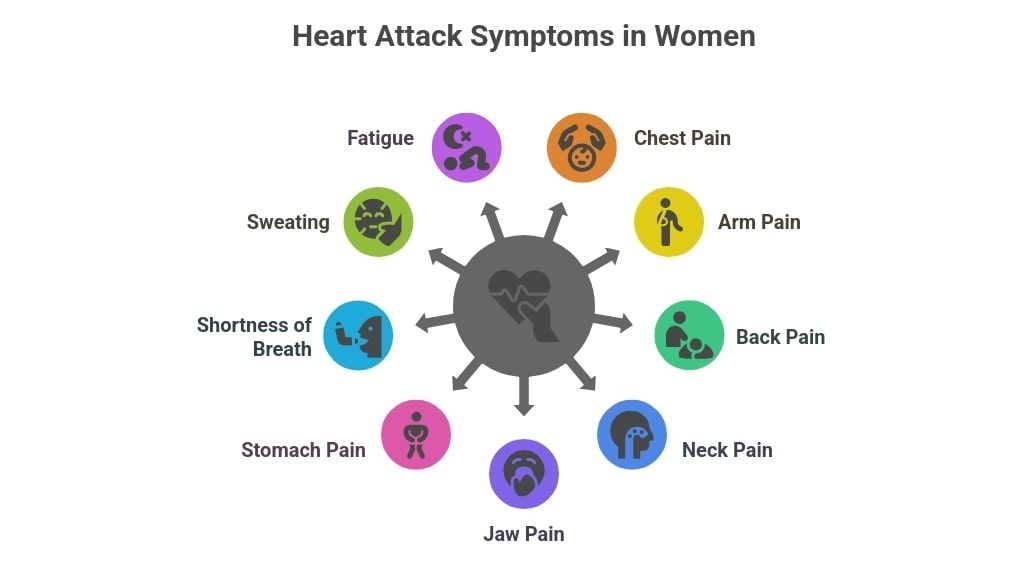
Women’s blood vessels are smaller, and plaque buildup often spreads differently. Hormonal changes after menopause also raise risk. Because early research centered on men, many guidelines and tests still do not catch women’s version of the disease as quickly. This gap leads to later treatment and worse results. Chronic conditions that affect women more than men are clearly seen in heart disease cases.
Also Read: Plantar Fasciitis: Causes, Prevention, And Home Treatment
Autoimmune Disorders
Women make up roughly 80 percent of people living with autoimmune diseases such as lupus, rheumatoid arthritis, multiple sclerosis, and Sjögren’s syndrome. Their immune systems are stronger overall, which helps fight infections but sometimes turns against the body itself. Women’s chronic diseases frequently involve autoimmune issues that disrupt daily life.

Scientists point to two main reasons. First, estrogen—the main female hormone—boosts immune activity. Second, women have two X chromosomes. One X chromosome stays partly active and can create proteins that the immune system sees as foreign, triggering attacks. These diseases often appear during the childbearing years when hormone levels are high. Diagnosis can take years because symptoms like fatigue and joint pain get dismissed as “normal” for women. Chronic pain conditions more common in women often overlap with these autoimmune disorders.
Also Read: Emerging Trends: Tech And Innovation In Women’s Health
Osteoporosis
After menopause, women lose bone strength faster than men. Estrogen protects bones, and its sharp drop causes rapid loss—up to 10 percent in the first five years. About 80 percent of the 10 million Americans with osteoporosis are women. One in two women over age 50 will break a bone because of it. Hip fractures are especially serious: many women never regain full mobility, and up to 25 percent die within a year. Women’s chronic diseases like osteoporosis highlight the long-term effects of chronic conditions on women’s health.
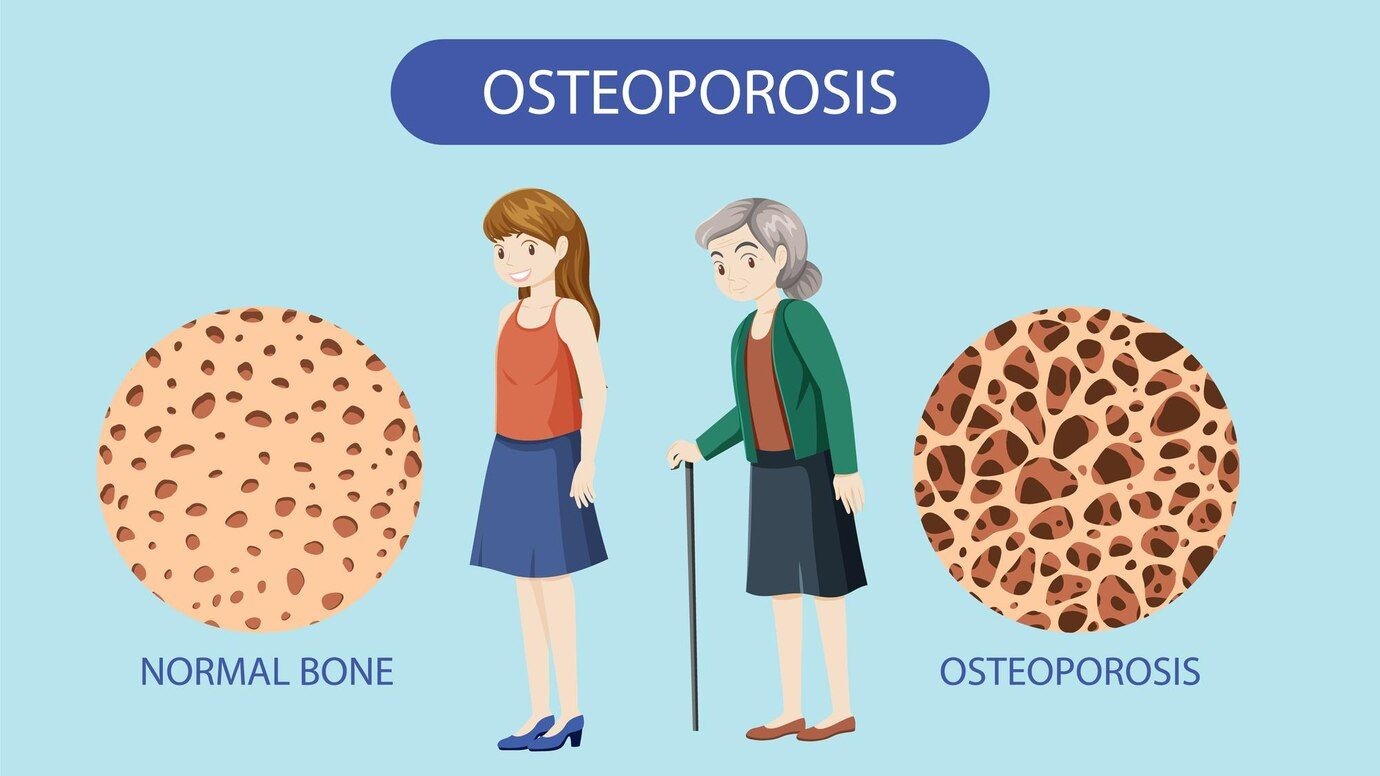
Family history, low body weight, and not enough calcium or vitamin D add to the risk. Yet many women do not get screened until after a fracture happens. Simple steps like weight-bearing exercise, calcium-rich foods, and doctor-recommended bone-density tests can help prevent it.
Alzheimer’s Disease
Nearly two-thirds of people with Alzheimer’s are women. The gap is not just because women live longer. The sharp fall in estrogen during menopause appears to play a direct role. Estrogen helps brain cells use energy and clear harmful proteins. When levels drop, the brain may switch to burning fats instead of glucose, and this shift can speed up the buildup of plaques and tangles linked to Alzheimer’s.
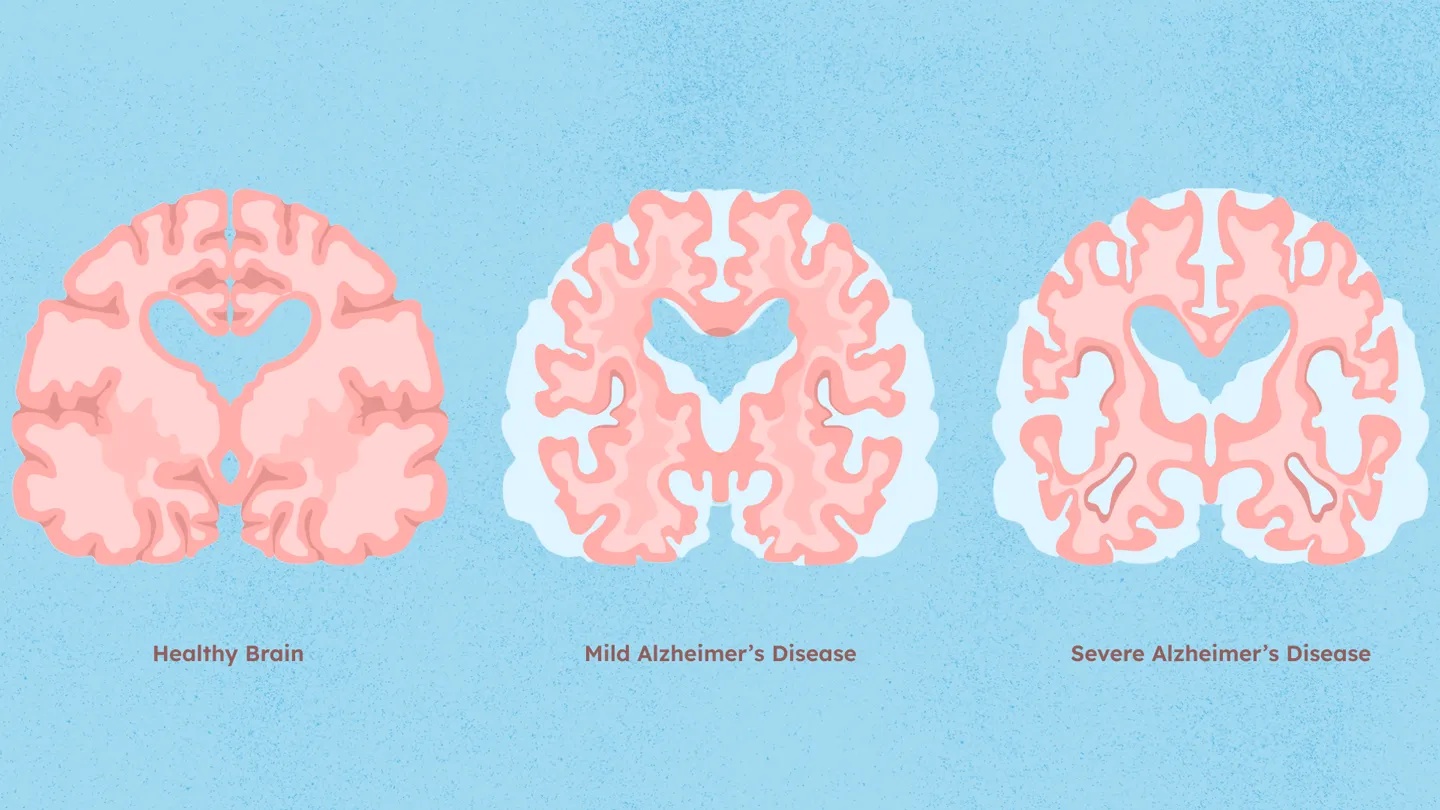
Women also tend to show more tau protein tangles in the brain, which hurts memory and thinking more severely. Lifestyle factors and genetics matter too, but the hormonal link is strong enough that researchers are studying whether timing hormone therapy carefully might lower risk in some women. Hormonal imbalances and chronic conditions in women play a key role here.
Also Read: Adolescent Girls’ Health – Early Pregnancy, Nutrition, And Rights
Metabolic Issues
Metabolic problems such as insulin resistance and type 2 diabetes affect women in unique ways. Polycystic ovary syndrome (PCOS), which strikes up to 10 percent of women of reproductive age, often brings severe insulin resistance—even in women who are not overweight. More than half of women with PCOS develop type 2 diabetes by age 40. Hormonal imbalances raise blood sugar, promote weight gain around the middle, and increase risks for heart disease later. Hormonal imbalances and chronic conditions in women create complex challenges in metabolic health.
Pregnancy can unmask these issues too. Gestational diabetes raises the chance of lifelong metabolic trouble. Because metabolic conditions interact with hormones, women’s bodies respond differently to diet, exercise, and medicine than men do. The long-term effects of chronic conditions on women’s health become evident in these ongoing metabolic struggles.
Why Research Bias Persists
For decades, medical studies treated the male body as the default. Until 1993, women of childbearing age were often kept out of clinical trials to protect unborn babies. Researchers worried that women’s monthly hormone changes would make results “messy.” Even after rules changed, many studies still do not analyze data by sex or include enough women. Funding for conditions that affect women more—such as endometriosis, migraines, or autoimmune diseases—remains low compared with the number of people who suffer.
This male-centered approach means doctors learn symptoms, drug doses, and test results based on men. Women’s different biology gets overlooked, leading to misdiagnosis and treatments that do not work as well. Bias also shows up in everyday care: women’s pain is more likely to be labeled as emotional rather than physical. Chronic conditions that affect women more than men often go under-researched because of this bias.
Promising Areas: Wearables and Better Monitoring
New technology offers real hope. Wearable devices that track metabolism and hormones are becoming smarter and more women-focused. Some patches and bracelets now measure hormones like estrogen, progesterone, cortisol, and even insulin-related markers through sweat or tiny fluid samples—without blood draws. Others combine heart-rate data, sleep patterns, and temperature changes to spot early signs of flare-ups in autoimmune disease or metabolic shifts during perimenopause.

These tools let women see daily patterns their doctors might miss in short office visits. Early studies show they can catch insulin resistance sooner, flag hormone drops linked to bone loss, and help tailor lifestyle changes or medicines. Researchers are also using artificial intelligence to turn wearable data into personalized alerts. While the devices are still improving, they point toward a future of prevention instead of late treatment. Women’s chronic diseases can be better managed with such advancements.
Also Read: Maternal And Newborn Health: Regaining Lost Ground
Moving Forward
Chronic conditions affect women differently for clear biological reasons, yet outdated research habits have left big gaps in care. Greater awareness, sex-specific studies, and user-friendly technology can close those gaps. When doctors, researchers, and women work together, earlier detection and better management become possible. The result is healthier lives for millions of women who deserve care that truly fits them. Chronic pain conditions are more common in women and the long-term effects of chronic conditions on women’s health deserve more attention moving forward. Women’s chronic diseases remain a critical focus for improving overall well-being.









