Why Women’s Hormones Affect Everything: A Complete Guide to Women’s Hormonal Health

A simple guide to understanding women’s hormonal health, at every age and stage of life.
Let’s start with something that might sound dramatic: hormones run the show. And nowhere is this more true than in women’s hormonal health.
Not in the way that dismisses your feelings as “just hormones,” that tired phrase that has been used to wave away women’s experiences for decades. Rather, it is meant in a very literal, biological sense. These tiny chemical messengers touch your mood, your sleep, your skin, your weight, your focus, your libido, your gut, and your heart. When they are in balance, you barely notice them. When they are not, it can feel like your body has turned against you.
The good news is that women’s health hormones are not a mystery reserved for doctors and researchers, and understanding them is one of the most useful things you can do for yourself. Once you understand what these hormones are and what they actually do, the symptoms that seemed random start to make sense, and so do the steps you can take.
So, What Exactly are Hormones?
Hormones are chemical substances produced by glands in your endocrine system. Think of them as messages: they are manufactured in one part of your body, released into the bloodstream, and then picked up by receptors in distant cells and organs, telling them what to do.
The tricky thing is that these systems are deeply interconnected. Your sex hormones influence your stress response. Your thyroid affects your mood. Your cortisol levels shape your blood sugar. Pull on one thread, and you often find it is attached to something else entirely.
For women, this complexity is even more layered because hormonal levels do not just vary from person to person. They change within a single month, shift across decades of life, and respond to things as ordinary as what you had for breakfast or how many hours you slept.
The Female Hormones That Shape Women’s Hormonal Health
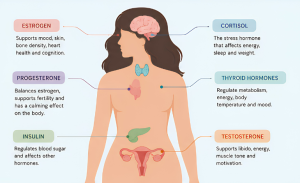
Without knowing about the female hormones that actually shape your hormonal health, would you be able to maintain and keep it in balance? No, right? Let’s talk about them below:
1. Estrogen
It’s the one that most people associate with being female, though its role goes far beyond reproduction. Estrogen supports bone density, skin elasticity, cardiovascular health, mood regulation, and cognitive function. It rises and falls predictably through the menstrual cycle, then gradually declines through perimenopause and menopause, making it central to women’s hormonal health at every stage. Of all the female hormones, estrogen has the widest reach, and its decline is felt across nearly every system in the body.
2. Progesterone
Progesterone is estrogen’s counterpart and a natural balancer. It is produced after ovulation and plays a central role in preparing the body for pregnancy. It also has a calming effect on the nervous system, which is why when progesterone levels drop, the effects are felt far beyond the reproductive system: anxiety increases, sleep deteriorates, and the second half of the cycle becomes noticeably harder.
3. Testosterone
Yes, women have testosterone too, just in smaller amounts. It matters more than many people realise. Testosterone influences libido, energy, motivation, muscle tone, and confidence. Levels naturally decline with age, and both PCOS and menopause can cause significant shifts.
4. Cortisol
Cortisol is your primary stress hormone, produced by the adrenal glands. In short bursts, it is genuinely useful as it helps you respond to danger and manage difficult situations. The relationship between cortisol and hormones like estrogen and progesterone is essentially competitive; when cortisol stays chronically elevated, the others get crowded out. Sleep suffers, fat accumulates around the abdomen, and the body’s ability to regulate itself gradually erodes.
5. Thyroid hormones (T3 and T4)
These hormones are produced by the thyroid glands, and they regulate your metabolism, body temperature, energy levels, and mood. Thyroid disorders, both underactive and overactive, are significantly more common in women than men and are frequently missed or misdiagnosed for years.
6. Insulin
Insulin is the hormone that controls how your body uses blood sugar. When cells become resistant to insulin’s signals (often due to diet, inactivity, or chronic stress), it can have significant downstream effects on other hormones. Insulin resistance is strongly linked to PCOS and can make weight management far harder than it should be.
How Female Hormones Change Across Life
Women’s hormonal health is not a fixed state. It is a moving landscape, shaped by age, biology, and circumstance.
The hormonal changes in women begin at puberty, when estrogen and progesterone surge, sometimes dramatically, triggering physical development and the beginning of the menstrual cycle. The mood swings that often comes with this phase is real, not imagined.
Through your twenties and thirties, hormones follow a more predictable monthly rhythm. However, stress, nutrition, travel, illness, and hormonal contraception can all shift that rhythm. Many women notice for the first time in their late twenties or early thirties that lifestyle choices have a very direct effect on how they feel across the month.
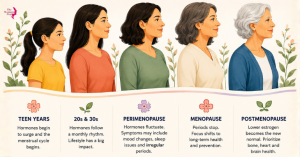
Of all the hormonal changes in women, perimenopause is perhaps the least talked about and the most disorienting. It can begin as early as the late thirties, but most commonly starts in the mid-forties, marking the beginning of a longer transition. Estrogen production becomes erratic rather than declining smoothly. Progesterone often drops earlier. This is when many women first experience hot flushes, disrupted sleep, mood changes, and a sense that their body is behaving unexpectedly.
Menopause refers to the 12 consecutive months that a women stays without periods. After this point, lower estrogen becomes the new normal, and the focus of women’s hormonal health shifts toward protecting bone density, heart health, and cognitive function over the longer term.
When Something Feels Off: Signs of Hormonal Imbalance in Women
The symptoms of hormonal imbalance in women are frustratingly non-specific. Many of them overlap with other conditions, which is part of why they are so often missed. That said, these are the most common signs you should pay attention to:
- Persistent fatigue that even sleeping doesn’t fix
- Weight gain that still continues even after diet or exercise changes
- Irregular, very heavy, or unusually painful periods
- Premenstrual syndrome (PMS) that feels unmanageable
- Skin breakouts in adults, especially around the jaw and chin
- Changes in hair such thinning on the scalp, or excess growth elsewhere
- Mood swings, anxiety, or low mood that tracks with your cycle
- Brain fog, poor concentration, or memory issues
- Low sex drive or vaginal dryness
- Sleep problems that feel distinct from ordinary stress
- Digestive changes, bloating, or shifts in appetite
One or two of these symptoms might have a simpler explanation. But if several appear together, or if they follow a cyclical pattern, it is worth taking seriously rather than pushing through. Recognising hormonal imbalance in women early makes a genuine difference to how quickly one can address it.
Most Common Women’s Hormonal Health Conditions
Few of the most common women’s hormonal health conditions include:
-
Polycystic ovary syndrome (PCOS)
PCOS is one of the most common hormonal disorders, affecting roughly 10-13% women of reproductive age though many go undiagnosed for years according to World Health Organization. At its core, PCOS is a hormonal imbalance, elevated androgens disrupt ovulation and drive a wide range of PCOS symptoms: irregular or absent periods, acne, excess facial or body hair, and difficulty managing weight despite no obvious dietary cause.
PCOS is also strongly linked to insulin resistance, which is why it tends to respond well to dietary changes and regular physical activity, as well as medical treatment. There is no single treatment that works for everyone, management is usually tailored to the person’s specific symptoms and goals.
-
Thyroid disorders
An underactive thyroid (hypothyroidism) slows everything down: metabolism, energy, digestion, mood. An overactive thyroid (hyperthyroidism) does the opposite. It causes heart palpitations, weight loss, anxiety, and heat sensitivity. Both are diagnosable with a blood test and very treatable. The challenge is that symptoms develop gradually and are easy to attribute to stress or ageing.
According to American Thyroid Association, women are more prone to developing thyroid disease (five to eight times more likely) than men, and autoimmune thyroid conditions (like Hashimoto’s) have a strong hereditary component. The connection between thyroid and hormones like estrogen is also bidirectional — estrogen affects how thyroid hormones are bound and used, which is why thyroid symptoms often worsen around the menstrual cycle and menopause.
-
Endometriosis
In endometriosis, tissue similar to the uterine lining grows outside the uterus, on the ovaries, fallopian tubes, bowel, or bladder. It is an estrogen-driven condition that causes significant pain, particularly around periods, as well as fatigue, bowel and bladder symptoms, and fertility difficulties.
Despite affecting roughly one in ten women, endometriosis is chronically underdiagnosed. The average time from first symptoms to diagnosis is still several years in many countries, largely because severe period pain has long been normalised rather than investigated.
-
Perimenopause
Perimenopause is not a single event: it is a transition that can span several years, sometimes beginning as early as the late thirties. Estrogen fluctuates widely before it finally declines, which is what makes this phase feel so unpredictable. Perimenopause symptoms: hot flushes, night sweats, sleep disruption, anxiety, brain fog, mood changes, and irregular periods are all common in this phase, but they are also frequently attributed to stress, burnout, or depression rather than hormonal change.
Understanding that perimenopause is happening is itself enormously helpful. It means you can name, track and address the symptoms instead of enduring it in confusion.
What Actually Affects Your Hormonal Balance?
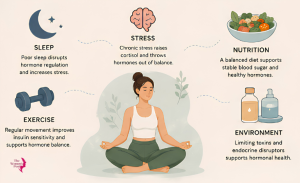
Hormones are not just determined by genetics or age. They are sensitive, dynamic, and responsive to everyday choices. Some of the most significant influences on women’s hormonal health include:
-
Sleep
Sleep is when the body regulates growth hormone, repairs tissue, and resets cortisol for the following day. Consistently poor sleep raises cortisol, disrupts insulin, and suppresses sex hormones. Even a few nights of broken sleep can have measurable hormonal effects.
-
Stress
Chronic stress is one of the most underestimated hormonal disruptors. When the body is in a prolonged stress response, cortisol remains elevated, and cortisol production competes with sex hormone production. This can suppress ovulation which results in irregular cycles. It can also dampen thyroid function.
The body prioritises short-term survival over long-term reproduction, and it shows. In cases of prolonged stress, the adrenal glands themselves can become depleted, a state often described as adrenal fatigue. This leaves women feeling exhausted even when nothing else is obviously wrong.
-
Nutrition
Blood sugar stability has a direct effect on insulin and, through insulin, on other hormones. Skipping meals, eating mostly refined carbohydrates, or following very low-calorie diets can all create hormonal turbulence. Equally important are nutrients like magnesium (involved in over 300 hormonal processes), zinc, vitamin D, and omega-3 fatty acids all commonly deficient in modern diets.
-
Exercise
Regular moderate exercise improves insulin sensitivity, reduces cortisol over time, and supports healthy estrogen metabolism. The caveat is that too much exercise without proper recovery, particularly in combination with undereating can suppress reproductive hormones significantly. Balance matters more than volume.
-
Gut health
The gut microbiome plays a role in how estrogen is metabolised and cleared from the body. An imbalanced microbiome can interfere with this process, leading to higher circulating estrogen levels, a pattern sometimes referred to as estrogen dominance, which is linked to heavier periods, bloating, and mood shifts. This is one reason why gut health and women’s hormonal health are increasingly understood as closely related.
-
Environmental exposures
Endocrine-disrupting chemicals found in certain plastics, pesticides, non-stick coatings, and many conventional personal care products can interfere with hormonal signalling. The evidence is growing, and while a single exposure is unlikely to cause harm, cumulative everyday exposure is worth thinking about.
How to Restore Hormonal Balance Naturally: A Guide to Women’s Health Hormones
Supporting women’s hormonal health is not always fully within our control. Hormonal changes in women are partly driven by biology and age, and some conditions require medical treatment. But there is also a great deal that lifestyle can genuinely shift. These are not quick fixes but they are habits that compound over time:
- Protect your sleep: Consistent sleep at consistent times has a larger effect on women’s hormonal health than almost anything else you can do.
- Eat to keep blood sugar stable: This means protein and healthy fats at every meal, fewer refined carbohydrates, and not skipping meals when stressed.
- Find a stress management practice that actually works for you: The evidence for breathwork, walking, yoga, and mindfulness on cortisol regulation is real.
- Move regularly, but recovery matters too: Strength training is particularly beneficial for insulin sensitivity and bone density.
- Reduce unnecessary exposure to plastics and synthetic fragrances: Small, consistent changes add up.
- Track your cycle and symptoms: Patterns become visible over time and that information is invaluable when speaking to a doctor.
- Ask for proper hormone testing: A comprehensive hormone panel blood test covering estrogen, progesterone, testosterone, thyroid markers, cortisol, and fasting insulin can reveal patterns a standard check-up will miss. Do not accept ‘everything is normal’ if something still feels wrong.
When to See A Doctor
Please do not wait until symptoms become severe before seeking help. It is worth making an appointment if you experience:
- Periods that stop for three or more months (without pregnancy)
- Extremely heavy bleeding or significant pain during periods
- PMS or PMDD that is affecting your work, relationships, or mental health
- Unexplained weight changes of more than a few kilograms
- Persistent fatigue, brain fog, or mood changes that do not have an obvious cause
- Signs of hormonal imbalance in a teenager that feel significant or distressing
Women’s hormonal health deserves to be taken seriously. Hormonal imbalance in women is one of the most underreported health concerns. Not because women do not notice, but because they are too often told it is normal. If something has changed and it is not resolving on its own, that is enough reason to seek support.
Frequently Asked Questions
These are the questions about women’s hormonal health we hear most often:
Can a hormonal imbalance in women cause anxiety and depression?
Yes, and this connection is more significant than it is often given credit for. Estrogen, progesterone, and cortisol all interact directly with serotonin, dopamine, and GABA, the neurotransmitters most closely associated with mood. When these hormones shift, particularly around the menstrual cycle, postpartum period, or perimenopause, mood disorders can emerge or become worse. This does not mean the anxiety or depression is not real. It means there may be a hormonal component worth addressing alongside any psychological support.
How do I know if I have PCOS?
PCOS is diagnosed based on at least two of three criteria: irregular or absent periods, elevated androgen levels (which might show up as symptoms like acne or excess hair, or in a blood test), and polycystic-appearing ovaries on an ultrasound. No single test confirms it, diagnosis involves ruling out other possible causes first. If you suspect PCOS, start with your GP, who can refer you to a gynaecologist or endocrinologist.
At what age does perimenopause usually start?
Most women begin perimenopause in their mid-to-late forties, though it can start as early as the late thirties. The transition typically lasts between four and eight years, though it varies considerably. Menopause, defined as twelve consecutive months without a period, occurs on average around age 51. Early menopause (before 45) and premature ovarian insufficiency (before 40) are less common but do occur, and both warrant prompt medical attention.
Can diet really make a difference to my hormones?
Genuinely, yes. Blood sugar levels influence insulin, which in turn affects sex hormones, cortisol, and appetite-regulating hormones. Nutritional deficiencies in magnesium, zinc, vitamin D, and omega-3s can impair hormone production. The gut microbiome shaped significantly by diet affects how estrogen is processed and cleared. None of this means diet is a substitute for medical care when a clinical condition is present. But it is a real lever, not a wellness myth.
Is HRT safe?
Modern hormone replacement therapy, particularly body-identical hormone therapy, is considered safe and effective. It’s increasingly understood as a key part of women’s hormonal health in midlife when prescribed and monitored appropriately. Earlier concerns about breast cancer risk were largely based on older synthetic formulations. Current evidence and clinical guidelines suggest that for women under 60 who are within ten years of menopause, the benefits typically outweigh the risks. The conversation has shifted significantly in recent years. A detailed discussion with a knowledgeable doctor, ideally one who specialises in menopause, is the best starting point.
Do hormonal contraceptives affect hormonal balance?
Hormonal contraceptives work by overriding the body’s natural hormonal cycle. For many women, this is straightforwardly useful. For others, synthetic hormones, particularly combined oral contraceptives can affect mood, libido, or nutrient levels, particularly B vitamins and magnesium. If you notice significant changes after starting or stopping hormonal contraception, those changes are worth discussing with your doctor rather than simply tolerating.
Can stress alone disrupt my cycle?
Yes, significantly. Cortisol, the primary stress hormone, competes with and suppresses reproductive hormones. Under sustained stress, ovulation can be delayed or suppressed entirely, leading to irregular or absent periods. This is not a dysfunction, it is the body rationally deprioritising reproduction when resources are stretched. The challenge is that modern stressors rarely resolve as quickly as the physical ones our hormones evolved to respond to.
Are hormonal problems hereditary?
Some aspects of women’s hormonal health are hereditary. The way female hormones are regulated has a genetic dimension, conditions like PCOS, autoimmune thyroid disease, endometriosis, and early menopause all tend to run in families. Having a family history raises your risk but does not guarantee you will develop the condition. More importantly, it is useful information, knowing your family history means you can watch for early signs, mention it to your doctor, and potentially catch things sooner.
This article is intended for general informational purposes and does not constitute medical advice. Women’s hormonal health is highly individual. If you have symptoms or concerns, please consult a qualified healthcare professional who can assess your specific situation.
Also Read:








